- Diabetes, obesity and metabolism
Big Data Articles (National Health Insurance Service Database)
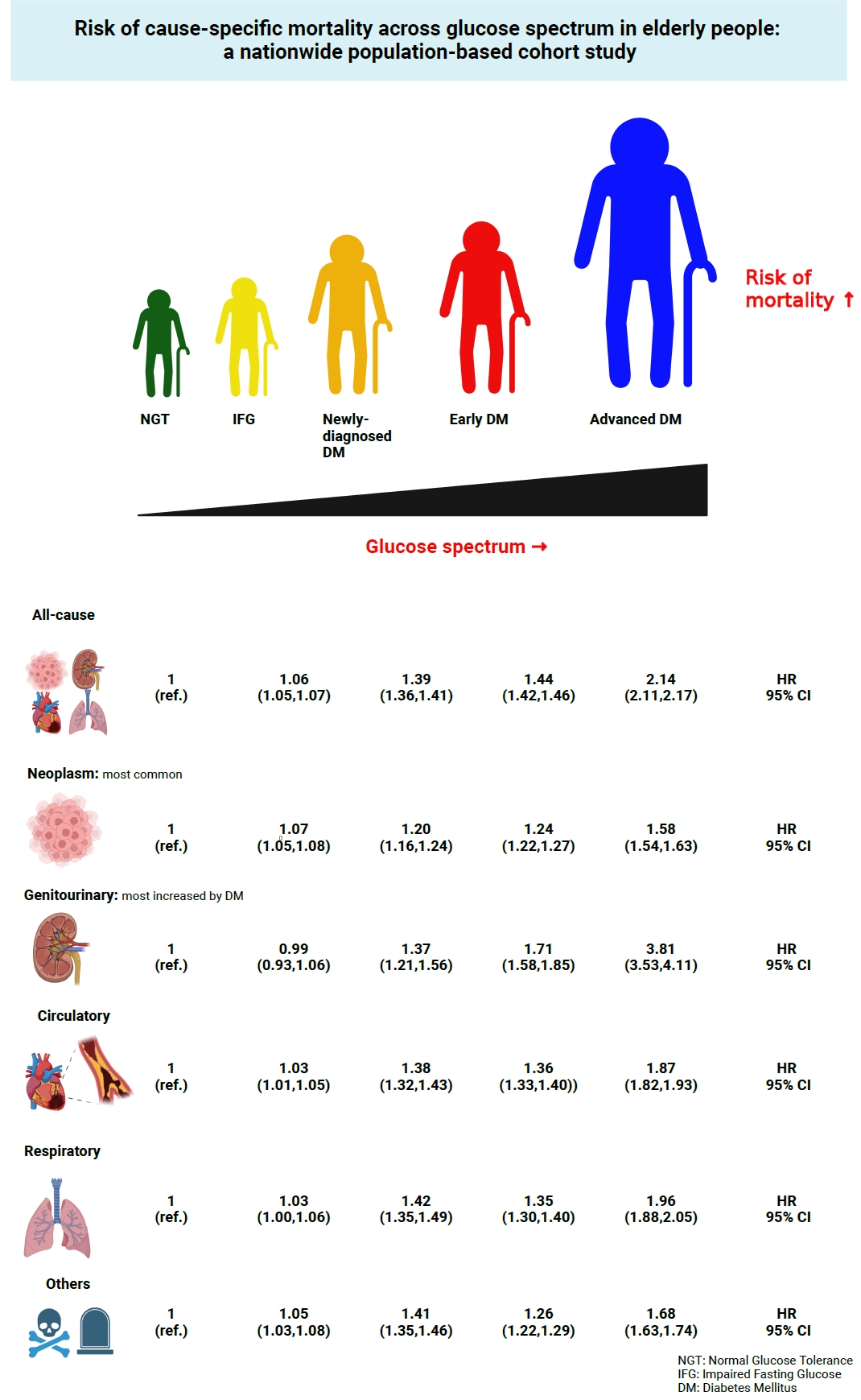
- Risk of Cause-Specific Mortality across Glucose Spectrum in Elderly People: A Nationwide Population-Based Cohort Study
-
Joonyub Lee, Hun-Sung Kim, Kee-Ho Song, Soon Jib Yoo, Kyungdo Han, Seung-Hwan Lee, Committee of Big Data, Korean Endocrine Society
-
Endocrinol Metab. 2023;38(5):525-537. Published online September 7, 2023
-
DOI: https://doi.org/10.3803/EnM.2023.1765
-
-
1,633
View
-
91
Download
-
1
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
This study investigated the risk of cause-specific mortality according to glucose tolerance status in elderly South Koreans.
Methods
A total of 1,292,264 individuals aged ≥65 years who received health examinations in 2009 were identified from the National Health Information Database. Participants were classified as normal glucose tolerance, impaired fasting glucose, newly-diagnosed diabetes, early diabetes (oral hypoglycemic agents ≤2), or advanced diabetes (oral hypoglycemic agents ≥3 or insulin). The risk of system-specific and disease-specific deaths was estimated using multivariate Cox proportional hazards analysis.
Results
During a median follow-up of 8.41 years, 257,356 deaths were recorded. Diabetes was associated with significantly higher risk of all-cause mortality (hazard ratio [HR], 1.58; 95% confidence interval [CI], 1.57 to 1.60); death due to circulatory (HR, 1.49; 95% CI, 1.46 to 1.52), respiratory (HR, 1.51; 95% CI, 1.47 to 1.55), and genitourinary systems (HR, 2.22; 95% CI, 2.10 to 2.35); and neoplasms (HR, 1.30; 95% CI, 1.28 to 1.32). Diabetes was also associated with a significantly higher risk of death due to ischemic heart disease (HR, 1.70; 95% CI, 1.63 to 1.76), cerebrovascular disease (HR, 1.46; 95% CI, 1.41 to 1.50), pneumonia (HR, 1.69; 95% CI, 1.63 to 1.76), and acute or chronic kidney disease (HR, 2.23; 95% CI, 2.09 to 2.38). There was a stepwise increase in the risk of death across the glucose spectrum (P for trend <0.0001). Stroke, heart failure, or chronic kidney disease increased the risk of all-cause mortality at every stage of glucose intolerance.
Conclusion
A dose-dependent association between the risk of mortality from various causes and severity of glucose tolerance was noted in the elderly population.
-
Citations
Citations to this article as recorded by  - The Characteristics and Risk of Mortality in the Elderly Korean Population
Sunghwan Suh
Endocrinology and Metabolism.2023; 38(5): 522. CrossRef
- Clinical Study
- Impaired Cortisol and Growth Hormone Counterregulatory Responses among Severe Hypoglycemic Patients with Type 2 Diabetes Mellitus
-
Young A Rhyu, Ju-Young Jang, Sooyoun Park, Jee Hyun An, Dong-Lim Kim, Suk Kyeong Kim, Kee-Ho Song
-
Endocrinol Metab. 2019;34(2):187-194. Published online June 24, 2019
-
DOI: https://doi.org/10.3803/EnM.2019.34.2.187
-
-
5,051
View
-
75
Download
-
10
Web of Science
-
12
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
Elevated levels of cortisol and growth hormone are critical counterregulatory responses to severe hypoglycemia. However, the proportion and clinical characteristics of patients with type 2 diabetes mellitus (DM) who fail to show appropriate cortisol and/or growth hormone secretion in response to severe hypoglycemia have not been investigated. MethodsWe measured plasma cortisol and growth hormone levels in type 2 DM patients with severe hypoglycemia who visited the emergency department between 2006 and 2015. ResultsOf 112 hypoglycemic patients, 23 (20.5%) had an impaired cortisol response (<18 µg/dL) and 82 patients (73.2%) had an impaired growth hormone response (<5 ng/mL). Nineteen patients (17.0%) had impaired responses to both cortisol and growth hormone. The patients with impaired responses of cortisol, growth hormone, and both hormones were significantly older and more likely to be female, and had higher admission rates, lower growth hormone levels, and lower adrenocorticotropic hormone levels than the patients with a normal hormonal response. Multivariate logistic regression analysis indicated that an impaired growth hormone response was significantly associated with advanced age, shorter DM duration, a higher admission rate, and a higher body mass index (BMI). An impaired cortisol response was significantly associated with growth hormone levels. Patients with an impaired growth hormone response had higher admission rates than patients with a normal response. ConclusionA considerable number of type 2 DM patients had impaired cortisol and/or growth hormone responses to severe hypoglycemia. Advanced age, shorter DM duration, and higher BMI were independently associated with an abnormal growth hormone response.
-
Citations
Citations to this article as recorded by  - The deleterious effects of sofosbuvir and ribavirin (antiviral drugs against hepatitis C virus) on different body systems in male albino rats regarding reproductive, hematological, biochemical, hepatic, and renal profiles and histopathological changes
Rana A. Ali, Eatemad A. Awadalla, Yahia A. Amin, Samer S. Fouad, Maha Abd-El Baki Ahmed, Mohammed H. Hassan, Emaad Abdel-Kahaar, Rehab H. Abdel-Aziz
Scientific Reports.2024;[Epub] CrossRef - Prediabetes and mild hepatosteatosis are associated with blunted cortisol response to glucagon but not to growth hormone
Ozlem Deveci, Zuleyha Karaca, Fatih Tanriverdi, Kamil Deveci, Aysa Hacioglu, Kursad Unluhizarci, Fahrettin Kelestimur
Annales d'Endocrinologie.2023; 84(2): 254. CrossRef - Evaluación del cortisol plasmático durante el test de ayuno en pacientes con síndrome hipoglucémico por hiperinsulinismo endógeno. Experiencia de 15 años
María Eugenia Gullace, María Victoria Ortuño, Teresa Mabel Canteros, Belén Bosco, Cintia Rodriguez, Javier Giunta, Lucas Costa, Andrea Kozak, Valeria de Miguel, Luis Grosembacher
Endocrinología, Diabetes y Nutrición.2023; 70(10): 634. CrossRef - Evaluation of plasma cortisol during fasting test in patients with endogenous hyperinsulinemic hypoglycemia. Fifteen years experience
María Eugenia Gullace, María Victoria Ortuño, Teresa Mabel Canteros, Belén Bosco, Cintia Rodriguez, Javier Giunta, Lucas Costa, Andrea Kozak, Valeria de Miguel, Luis Grosembacher
Endocrinología, Diabetes y Nutrición (English ed.).2023; 70(10): 634. CrossRef - Cerebrospinal fluid levels of hypothalamic-pituitary-adrenal axis hormones in MCI and dementia due to Alzheimer’s disease: a systematic review
Felipe Duarte-Zambrano, Jorge A. Barrero, Ismena Mockus
Dementia & Neuropsychologia.2023;[Epub] CrossRef - PTEN Deletion in Adult Mice Induces Hypoinsulinemia With Concomitant Low Glucose Levels
Maria Crespo-Masip, Aurora Pérez-Gómez, Carla Guzmán, Sandra Rayego, Nuria Doladé, Alicia García-Carrasco, Ramiro Jover, José Manuel Valdivielso
Frontiers in Endocrinology.2022;[Epub] CrossRef - Beta Blockers can Mask not only Hypoglycemia but also Hypotension
Goran Koracevic, Sladjana Micic, Milovan Stojanovic, Radmila Velickovic Radovanovic, Milan Pavlovic, Tomislav Kostic, Dragan Djordjevic, Nebojsa Antonijevic, Maja Koracevic, Vesna Atanaskovic, Sonja Dakic
Current Pharmaceutical Design.2022; 28(20): 1660. CrossRef - Atherosclerosis Risk Factors in Patients with Reactive Hypoglycemia
Małgorzata Landowska, Agata Żebrowska, Konrad Fajer, Patrycja Adamek, Aleksandra Kruk, Bernadetta Kałuża, Edward Franek
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2022; Volume 15: 3133. CrossRef - Depression with Comorbid Diabetes: What Evidence Exists for Treatments Using Traditional Chinese Medicine and Natural Products?
Yanting Lu, Tao An, Hu Tian, Xueqin Gao, Furong Wang, Shijun Wang, Ke Ma
Frontiers in Pharmacology.2021;[Epub] CrossRef - Hepatocyte-specific glucose-6-phosphatase deficiency disturbs platelet aggregation and decreases blood monocytes upon fasting-induced hypoglycemia
Anouk M. La Rose, Venetia Bazioti, Joanne A. Hoogerland, Arthur F. Svendsen, Anouk G. Groenen, Martijn van Faassen, Martijn G.S. Rutten, Niels J. Kloosterhuis, Bertien Dethmers-Ausema, J. Hendrik Nijland, Gilles Mithieux, Fabienne Rajas, Folkert Kuipers,
Molecular Metabolism.2021; 53: 101265. CrossRef - Effects of tofogliflozin on adrenocorticotropic hormone, renin and aldosterone, and cortisol levels in elderly patients with diabetes mellitus
Toshihiro Higashikawa, Tomohiko Ito, Takurou Mizuno, Keiichirou Ishigami, Kengo Kuroki, Naoto Maekawa, Daisuke Usuda, Takuro Morita, Kazu Hamada, Susumu Takagi, Kento Takeshima, Shinya Yamada, Ryusho Sangen, Toshihide Izumida, Hideyuki Mori, Jun Kiyosawa,
Medicine.2021; 100(45): e27638. CrossRef - Stress, glucocorticoid signaling pathway, and metabolic disorders
Roldan M. de Guia
Diabetes & Metabolic Syndrome: Clinical Research & Reviews.2020; 14(5): 1273. CrossRef
|